Ania's Medial Meniscus Surgery
November 1, 2005
People write stories of their adventures in distant lands among foreign cultures. This is one of mine. I travelled a mile from home to the University of Washington Surgery Pavilion.
The night before: Monday night, I puttered around the house getting everything ready. I did laundry. I picked out post-surgery reading material. I bought bagels. I checked the fridge to make sure my frozen dinners were still in place. I reminded myself that my surgery the next day was a routine procedure, that I'd never had an averse reaction to any drug, and that healthy young people like myself tend to recover quickly. Finally, I admitted that I was simply stressing needlessly. I called Seth and we went out for my "last supper" before surgery to get me out of the house.
So small:
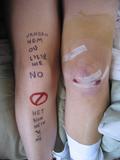
The nurses know the rules: One nurse gave me a hospital gown, which I put on backwards as it later turned out. Another nurse asked me the same questions I'd already answered several times: name, date of birth, allergies, and do I have any jewelry, dentures, or contact lenses. A third nurse wrote his initials on my left leg, which is how they identify the limb to be operated. He was unamused by my long list of NOs and sternly warned me that the staff might confuse my decorations with his initials. The next day in my post-op visit, Dr. Larson laughed at the list. While he admitted that it was against procedure, he thought it unlikely that the universal red circle with a diagonal red slash would be misinterpreted for initials. | 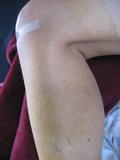
| 
|
| The nurse's initials (look carefully near bottom of image) | Ania's joke. Apparently, not funny. |
Arduous struggle: Finally came my one challenge of the day. I had anticipated this moment and had mentally rehearsed how I would be calm and firm in the face of scary propaganda intended to change my mind. Alan, the nurse anesthetist, came in to discuss anesthesia. Knocking out the patient makes the procedure more predictable and thus easy and efficient for the staff so he recommended general anesthesia. I wanted to stay awake which would necessitate an alternative to general anesthesia. I noted that Dr. Larson had said it would be alright for me to stay awake. Alan countered by emphasizing the ease and safety of generals. He proceeded to threaten me with a 5% risk of a spinal headache if I got a spinal. If too much cerebro-spinal fluid (CSF) leaks out, the patient may get a headache worse than a migraine, treatable only by laying flat for two days. He emphasized increased risk with out-patient surgery since I'd need to move to get into a car or around my house, and motion increases risk of CSF leakage. He then explained that other alternatives, a sciatic nerve block or an epidural, were complicated and he would not do either of those on me. My choices were thus a spinal with the risk of the dreaded spinal headache or the safe and easy general. I stood my ground and bravely stayed with my original request of a spinal.
Meet the anesthesiologist: Then a jolly older man wandered into the room. It turns out he was the anesthesiologist. He grinned and told me that a spinal was the best choice for this surgery. I laughed and gave Alan a look of "I told you so." Alan looked at me seriously and said that the anesthesiologist was wrong. I said I believed them both and would still like a spinal. The anesthesiologist said nothing, continued to smile, and blithely meandered away.
They didn't knock me out! Alan rolled me to surgery. He introduced me to Arnold, a nurse who'd be assisting in the surgery. They helped me sit up and painted my back with betadine. Dr. Larson, my surgeon, was nowhere to be seen so Alan had Arnold go find him. With the surgeon on his way, Alan had me round my back and injected lidocaine into my cerebrospinal fluid. The anesthesiologist chattered instructions and suggestions throughout this procedure, which Alan seemed to mostly ignore. Arnold and Alan hurried to get me situated on the operating table before my lower body went numb and I wouldn't be able to help. A drape went up to isolate my sterile leg, yellow with betadine, from unsterile me. Arnold moved one of three monitors to my side so I'd be able to observe everything that the arthroscopic camera saw. Alan gave me a shot of something "to relax me" which thankfully seemed to have no effect. I carefully did not comment, in case Alan should deem it helpful to give me more.
Arthroscopic surgery rocks: With the arthroscopic camera view and Dr. Larson's occassional comments, I felt I understood what went on. It was interesting. It also seemed straightforward, obvious, and simple, which is how complex procedures appear when accomplished by well-practiced experts. Once the torn piece of cartilage had been removed, Arnold brought it around for me to see. The only disquieting part of the procedure was that I could feel pressure on my leg and had some proprioception. I felt no pain but felt pressure when each arthroscopic instrument was initially inserted. I also felt my leg being moved and slightly torqued to give Dr. Larson better access to one side of the joint or the other. Time flew quickly, as it does when one is having fun.
Julia, the nurse: Alan wheeled me from surgery to a recovery room. There, I met Julia. She was a friendly, intelligent woman and we had wonderful conversation for the couple of hours before my spinal wore off. She told me how being 7.5 months pregnant affected her job as a nurse, of going on rounds with her father who was a doctor, of her mathematician husband who was not always thrilled to be included in sometimes gruesome dinner conversations that Julia's medically-inclined family enjoyed, how to read my EEG, and what drugs I had been given and why. We shared our previous experiences with spinals. She didn't object to me holding my breath to make my oxygen level drop on the monitor. When I brought her running into my room by seeing what would happen to the monitors if I started hyperventilating, she took my explanation entirely in stride and didn't seem surprised. When I told her I was a little cold and shivering but not hypothermic and assured her that I knew how hypothermia felt, she took my temperature nonetheless but laughed and commented that "you never know what your patients are going to say." It was a first class facility. In fine hotels, the staff launders your sheets and brings you food. Julia likewise brought me juice and cheese and crackers, and reassured me not to worry about making a mess. She went a step further than the finest hotels, however. She even peed for for me. What service! When I suggested that my bladder might be full but noted that I didn't have the muscular control to pee yet, she brought out a sonographic gizmo to verify the fullnes of my bladder. Imagine telling someone 100 years ago that we'd have tools to diagnose whether you need to pee! At my request, she inserted a catheter to drain my bladder, with no effort on my part. I've never heard of a hotel that so fully pampers its guests. Then she told me the story of a king's personal physician who died after his bladder burst. The physician liked to drink and it was impolite to leave the dining room while the king was present, so he postponed peeing just a bit too long and the world lost a great physician.
Daisy the Crazy: Julia's shift was over but my spinal wasn't, so Daisy came in to take over. Julia and I jokingly retold Daisy how I'd held my breath to see what the monitor would do. Daisy said she'd smack me if I did that on her shift. I promptly held my nose and stopped breathing. She responded by taunting me that I had dribbled cracker crumbs on myself. I pointed out that it was her job to clean up after me. She bent over and huffed a big puff of air at me to blow them off. A third nurse happend to be passing by and, surprised by Daisy's entirely unprofessional action, asked whether we knew each other. I replied that no, we'd just met. Julia, Daisy, and I all burst out laughing. When Julia, Daisy, and I were alone again, I commented on my anesthesiology staff. I said that Alan (the nurse anesthetist) had seemed competent and knowledgable. In contrast, I couldn't tell whether the anesthesiologist was just there because an anesthesiologist had to be present, or whether under that carefree demeanor he actually had a lot of knowledge and experience. The nurses looked at each other for a moment. Then one said: "No comment. I think that's all we can say. No comment."
Drugs: The doctor's assistant came by to prescribe me painkillers to take home. I said I'd never tried Percocet (oxycodone and acetaminophen) and was wondering whether he could prescribe me both that and Vicadin (hydrocodone and acetaminophen) so I could compare. He replied that prescribing me multiple narcotics would send off a red flag at the pharmacy. Furthermore, taking both at once was not recommended. Since I'd never had Percocet, he prescribed me that for pain and ibuprofen for swelling. He added that Percocet can cause stomach upset, so if I didn't tolerate it well, to call the clinic and they could phone in a prescription for Vicadin.
They're smart: It's quite clear to me that doctors and nurses both do a lot of unspoken patient assessment. They make judgements on whether a patient is likely to get hooked on or abuse the drugs they are being given. They assess whether a patient seems to understand the instructions they are given for going home. They assess whether the patient will have adequate care once they get home. While it's sometimes fashionable to speak of Western medicine as not holistic, the staff who cared for me were clearly looking at me as a whole person, not just a damaged knee with 125 lbs of attached flesh.
A nice day: When Lauren arrived to pick me up, I was quite cheerful. I'd had a painfree morning of medical education and interesting conversation. Alan had been patient and pleasant, and thankfully did not make me dopey with drugs. Julia had provided great conversation and entertainment during recovery. Dr. Larson had done his job just as a very competent mechanic services a car: quickly, efficiently, reliably. Amy, a housemate's girlfriend, had suggested I wear a skirt to the hospital, which made getting dressed easy in spite of the dressing around my knee. When we got home, to my surprise I had no trouble walking from the car and up the steps into our house. Lauren helped me settle down on a couch, brought me tea, and rented a movie that we watched together. She provided all the comforts of being mothered without any of the worrying and lecturing that a real mother surely would have exuded. I felt great. Local anesthetics in my knee (lidocaine and morphine, plus epinephrine to keep them from washing out) kept the pain away, and since I had had only a minimal amount of drugs injected into my bloodstream I was fully coherent.
Amazingly fast recovery: Before going to sleep, I popped a Percocet. I still had no pain. I took it prophylactically, in case the local anesthetics in my knee wore off in the night. I woke up on Wednesday still free of pain. At my 9am doctor's appointment, a nurse removed my dressing. They recommended continuing to ice and elevate but were impressed with how minimally the leg was swelling. They also said that I had much greater range of motion than is typical for the day after surgery and gave me exercises to do every hour for further improvement. Two exercise sessions later, less than 24 hours after surgery, I could fully straighten my leg and could touch my heel to my butt. I'm to take it easy for a week so the incisions can heal but could be back to 100% of my activities within 2 weeks. Lauren thinks that my positive attitude had a lot to do with the quick recovery. I think receiving a minimal amount of drugs to make me spacey and actually following instructions (ice, elevate) helped. I'm also indebted to my wonderful support network of friends and housemates who kept company, brought me food, gave me rides, and generally offered help. In any case, modern orthopedic medicine is amazing.
Conclusion: I can recommend the UW Medical Center as a great place to take your next surgical vacation.
But seriously: I had a really good day. While my story above recounts some humorous anecdotes, I feel it only fair to be clear that I believe myself to have been well-cared for by competent staff at a well-run clinic. Both the staff of the University of Washington Surgery Pavilion and the doctors and nurses from UW Sports Medicine who actually performed my surgery did their jobs well. They were clearly careful to follow routine safety procedures. Everyone was willing to answer all my questions fully. I was treated with respect and care for my entire person. Alan clearly presented the pros and cons of my anesthesia choices and respected my decision. He exuded an attitude of calm, control, competence, and respect for the patient. Julia was not only full of amusing stories but also clearly knowledgable and competent in the execution of that knowledge. Daisy's sense of humor was appropriate for me, since I responded equally in jest. My meetings with Dr. Larson were brief and few, but all my questions were answered. He respected my desire to have a full understanding of what is going on, likely to a much greater detail than most patients. I appreciate him granting my request to stay awake, the anatomy lesson I received in my pre-op appointment, his explanations of what I was seeing on the screen during surgery, and the photographs he took during surgery that he gave me the following day. His ability to answer all my questions and the efficiency with which he performed the surgery are consistent his great competence as a surgeon.
Other links:
Read about my next surgery: Last updated 7 April 2006 © Anna Mitros
Back to Ania's Home Page